13 Sep Lymphoma
 Lymphoma
Lymphoma
This month it is World Lymphoma day-but what is lymphoma and how can it affect your body and your skin?
What is lymphoma?
Lymphoma is a type of blood cancer, it is the fifth most common cancer in the UK and can affect people of any age. Blood cancers develop when the growth of blood cells is out of control, they may divide abnormally or fail to die when they are damaged causing abnormal cells to build up in the circulation.
Lymphoma got its name because it is a cancer of the lymphatic system, the network of vessels and nodes that are a vital part of the body’s protection against disease. Lymphoma develops when white blood cells called lymphocytes begin to divide and grow abnormally. Lymphocytes are an important part of the immune system that helps us detect abnormal cells or infections and fight illness. In lymphoma abnormal lymphocytes build up in the body. They often collect in the lymph nodes, causing lumps and swellings in the neck, armpits or groin.
As lymphoma develops, the abnormal cells can spread through the lymphatic system, or through the bloodstream to the lungs, liver or bone marrow. The body can be overwhelmed by lymphoma cells, which impact on the body’s ability to function normally. However, the good news is that most lymphomas are treatable, with people usually living for many years after diagnosis.
Types of lymphoma
There are more than 60 different types of lymphoma, which can cause different symptoms and respond to different treatment regimes. Lymphomas are divided into two groups: Hodgkin lymphomas and non-Hodgkin lymphomas. The main difference is the type of lymphocyte involved and their appearance under the microscope. If an abnormal cell, known as a Reed-Sternberg cell, is present the lymphoma is classified as Hodgkin’s disease. Lymphoma can affect any part of the body including the skin.
What causes lymphoma?
Frustratingly, we don’t fully understand the causes of lymphoma, however we know that there are a number of factors that increase your risk of developing the disease.
Lymphoma is more common in people with weaker immune systems, for example due to medication or HIV, and in people living with autoimmune conditions. Radiation, some agricultural chemicals and breast implants have also been linked to some types of non-Hodgkin lymphoma. Certain infections may increase the risk of developing the disease, the Epstein-Barr virus that causes glandular fever has been particularly implicated in both non-Hodgkin and Hodgkin types. There also appears to be a genetic link, as there is a high risk of getting Hodgkin lymphoma if a twin has the disease.
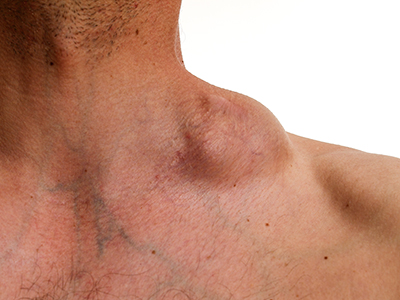 What are the symptoms of lymphoma?
What are the symptoms of lymphoma?
The symptoms of lymphoma depend on the type of lymphoma, the part of the body affected and the stage of the disease.
The main symptom of lymphoma is swollen lymph glands. You may notice a lump in the neck, armpit or groin where the nodes are near the surface of the skin. If the glands are deeper in the body they cannot be seen or felt, instead you may notice symptoms caused by the swollen node pressing on other structures. These can include bone pain, breathlessness and chest or abdominal pain.
Lymphoma can also cause more general symptoms, known as ‘B symptoms’. These include fever, night sweats and unexplained weight loss, the presence of which can affect the type of treatment required.
Your skin and lymphoma
Skin lymphoma is a rare type of lymphoma that causes skin rashes and lumps and develops in the skin. It’s usually a low-grade lymphoma, but it can be missed because it can be mistaken for other skin diseases including eczema or psoriasis. The rash of cutaneous lymphoma can appear as:
- Flat pink or red patches which can be dry and itchy
- Thickened skin with raised scaly plaques, which can itch or become ulcerated
- Lumps in the skin
Anyone who has a rash that doesn’t resolve, is spreading rapidly, is affecting normal life or is linked to breathlessness, fever or malaise should see their doctor.
Managing skin symptoms of lymphoma
Many skin lymphomas are slow growing and unlikely to affect life expectancy, however they can be uncomfortable and unsightly. If your doctor has advised a ‘watch and wait’ strategy for managing your lymphoma, there are ways to ease discomfort and soothe your skin:
- Ease itching: Cold compresses, steroid creams or lotions with 1% menthol can cool and soothe itching.
- Apply emollients: Emollients are topical treatments that moisturise the skin, preventing dryness. The AproDerm® Emollient Cream forms a protective layer over the skin, trapping in water and rehydrating the cells. Regular use of an emollient can help relieve tightness, scaling and discomfort and can ease any itching.
- Minimise skin irritation: Wear comfortable clothes in natural fabrics and avoid harsh detergents and chemicals that can sensitise and irritate the skin. The AproDerm® range is scientifically formulated to be free from SLS, parabens, halogens, fragrances and colours to decrease the danger of inflammation.
- Treat infections: If the skin becomes more red, hot or swollen or if there is any pus or discharge present there may be an infection, which needs prompt medical assessment and treatment.
- Oatmeal is a traditional remedy for skin dryness. Colloidal oats moisturise the skin, helping to reduce roughness and scaling. AproDerm® Colloidal Oat Cream is formulated with active colloidal oatmeal, which protects and restores the skin’s surface.
- Tepid bathing: Hot baths can strip the skin of moisture. Use lukewarm water when bathing, avoid soaps and afterwards smooth an emollient onto your damp skin.
- Stay cool: Inflamed skin can be hot and painful. Wear light, loose clothes in natural fibres and turn the heating down a notch. Drink plenty of fluids to stay hydrated, use paracetamol to stay comfortable and apply emollients regularly to moisturise the skin and reduce transepidermal fluid loss. If you’re developing a high fever, feeling weak or unwell see your doctor, you may need medical support and treatment in hospital.
- Look after yourself: Living with a serious chronic condition can have a serious impact on your wellbeing and confidence. If you are worried about the appearance of your skin, camouflage creams can help. Talk to your medical team about products that won’t cause irritation. Changing Faces is a charity that provides a free skin camouflage service as well as providing support for people living with scars, disfigurement or skin problems.



Sorry, the comment form is closed at this time.